|
Anticonvulsant
Guidelines |
The results of the MAGPIE and Collaborative Eclampsia Trials indicate that magnesium sulphate is the drug of choice for the prophylaxis and treatment of eclamptic seizures. All women who meet the inclusion criteria should be treated with magnesium.
|
Initial Treatment (Loading Dose) |
2 g (20 ml) 10% MgSO4 infused
IV over 5 mins, then further 2 g (20 ml) MgSO4 infused over 10 mins,
then |
|
Maintenance Dose |
1 g (10 ml) / hr IV 10% MgSO4 |
(This volume needs to be deducted from the hourly maintenance fluid)
| Contraindications | with severe cardiac disease or acute renal failure use 10 mg Diazemuls then 2.5 mg / hr |
| Duration of Infusion | while patient is on Delivery Suite (i.e.) 24-48 hrs |
| Monitoring | Clinical: hourly patellar reflexes after the loading dose. Use arm reflexes in presence of an epidural. |
Magnesium Levels
Experience from the Collaborative Eclampsia Trial indicates that MgSO4 administered according to the above regimen can be used safely without the need to monitor Mg levels. Mg is excreted by the kidneys and toxicity is more likely if there is oliguria (urine output < 100 ml / 4 hrs) or urea > 10 mmol / L. Measurement of Mg levels may facilitate care however where there are signs of toxicity.
Toxicity
Signs of toxicity are extremely uncommon and correlate with magnesium levels.
Therapeutic Range loss of tendon reflexes, weakness, nausea, feeling of warmth, flushing, somnolence, double vision, slurred speech muscle paralysis, respiratory arrest cardiac arrest Patellar reflex and oxygen saturation MUST be recorded on the PET chart. If the midwife is to carry out clinical monitoring, the SHO should ensure these are performed and recorded adequately.
Loss of patellar reflex Stop maintenance infusion
If possible, check Mg level
Withold further Mg until patellar reflexes return or Mg
levels known Oxygen saturation persistently < 92% Commence O2, check patellar reflexes, inform anaesthetist If patellar reflexes present, exclude other causes (eg) opiates,
pulmonary oedema
If patellar reflexes absent, see above.Cardiorespiratory arrest Stop maintenance infusion
Institute CPR
Administer 10 ml Calcium gluconate IV
Intubate immediately and manage with assisted ventilation
until resumption of spontaneous respirations
If possible, check Mg levelsSeizure on Magnesium Treat seizure with a further bolus of Mg 2 g over 5 minutes
If possible check Mg levels prior to this
If further seizures despite this, consider:
Diazemuls 10 mg IV bolus then infusion
Thiopentone infusion on ITU Once tendon reflexes return, if Mg level < 4 mmol / L restart maintenance dose at 0.5 g / hr and recheck levels in 3 hours.
If Mg level < 2.0 mmol / L restart maintenance dose at 2 g / hr.
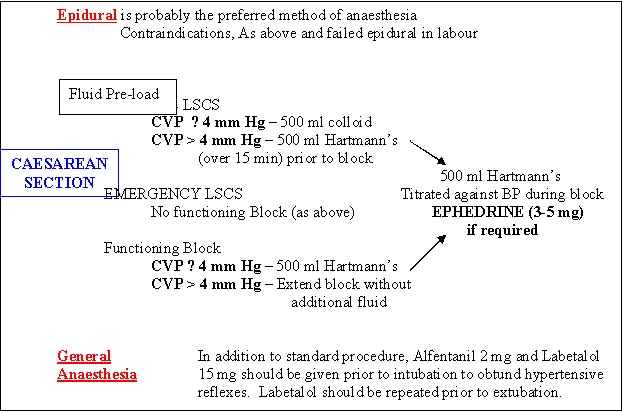
LABOUR Epidural is the preferred method of analgesia
Contraindications; Platelet count < 80x 109 /l
Elevated APTT or TT, Maternal refusalFluid Pre-load; 500 ml Hartmann's (over 15 min) prior to block
Thereafter continue on Hartmann's (1 litre/12h) unless oliguric
CRITERIA FOR CONSIDERING TRANSFER TO ITU 1. Recurrent seizures
2. MAP > 125 mm Hg despite IV hydralazine & Labetalol
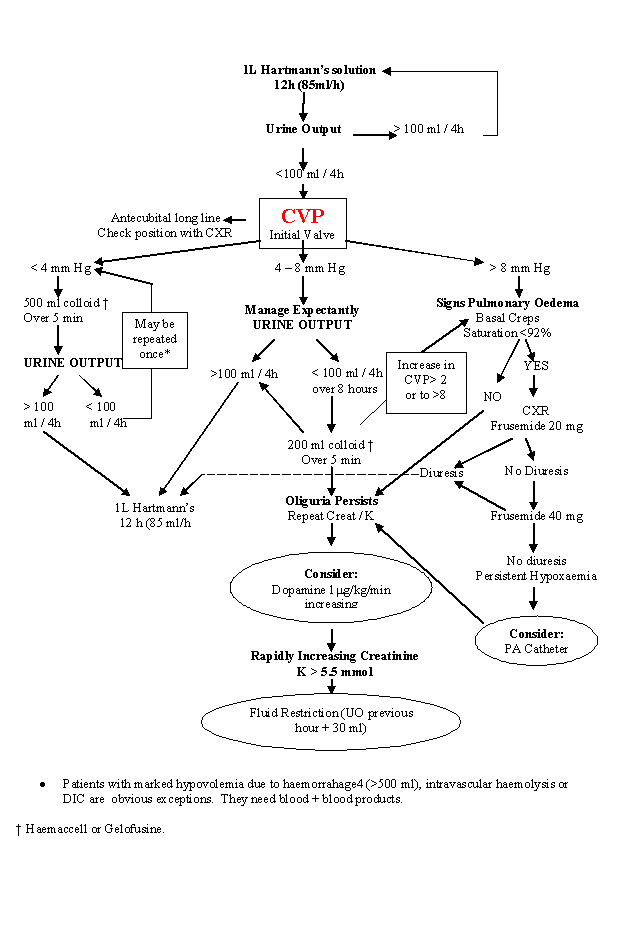
3. Persistent oliguria with normal / high CVP
4. Pulmonary oedema with oliguria
5. Compromised myocardial function
MAPs > 140 mm Hg constitute an obstetric emergency
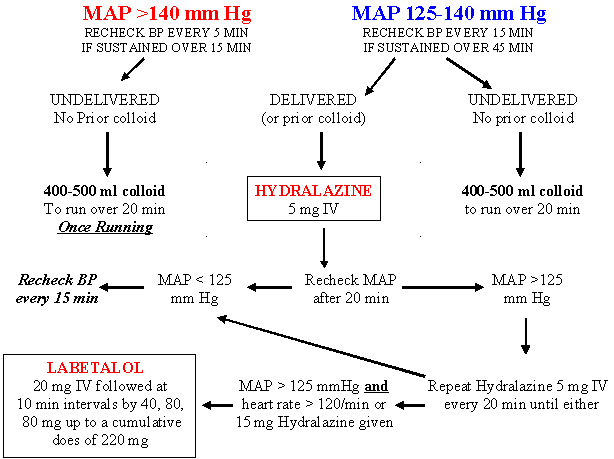
Subsequent episodes of hypertension can be managed with intermittent IV bolus therapy
(hydralazine 5 mg or Labetalol 40 mg) but if these are required more than once / hour consider an infusion:
HYDRALAZINE
LABETALOL
Only women with severe PET/eclampsia will be managed according to the guideline.
All women will remain on labour ward for a minimum of 24 hours after delivery.
Please ensure that when the patient is transferred to the PN ward the ward staff are made aware of the need for strict fluid balance for at least 48 hours.Aspects of Care
1 PET charts: These should be filled in HOURLY ie at 8am, 9am etc. Record the hourly fluid intake (IV & oral), urine output & fluid balance, BP, CVP, oxygen saturation & reflexes (whilst on magnesium). Remember to fill in important events ie antihypertensive treatment, epidural insertion, top ups, delivery and mark delivery BLOOD LOSS. 2 BP measurements: Automatic sphygmomanometers may underestimate BP.
It is necessary to validate automated measurements against standard mercury sphymomanometry at the beginning of monitoring and intermittently (e.g. every 2 hours) thereafter. BP measurements should be made every 15 minutes and recorded on the PET chart. Inform the SHO if there are two consecutive readings with MAP >125 mm Hg or one reading >140 mm Hg.3 Fluid intake: The standard IV fluid regime is 85 ml/hour. This includes the 20 ml of magnesium each hour (ie women on Mg will be on 65 ml Hartmann's/hour). Once oral fluids are established the hourly oral intake needs to be subtracted from the IV input (if a women is drinking 50 ml/hour she needs approx. 35 ml/hr IV). 4 Urine output: This is measured hourly using the calibrated meters. Inform the SHO if the output is <100 ml over a FOUR hour period. 5 CVP: This is recorded hourly. The anaesthetist is responsible for the insertion and subsequent care of the CVP line. If you have any concerns regarding measurement then inform the anaesthetist. If the CVP is >12 cm inform the SHO. 6 Magnesium sulphate: The drug is given by IV infusion. The first signs of toxicity are loss of tendon reflexes & respiratory depression. Therefore throughout the infusion hourly recordings must be made of;
a) Patellar reflex; The method of testing the patellar &/or biceps reflex will be explained by the SHO. If you fail to detect a reflex or are unhappy about the method of testing you must let the SHO know immediately; it is their responsibility to teach you!
b) Oxygen saturation; Inform SHO if persistently < 90%7 Cord gases: Every attempt must be made to get arterial & venous samples and complete results should be recorded in the delivery notes.